Lichen Planus
WHAT IS LICHEN PLANUS?
EPIDEMIOLOGY
The disorder affects about one in one hundred people around the world, being mostly prevalent among adults over the age of 30. Accordingly, it is very rare in children. In about 10% of cases significant family history has been noted, making it one of the predisposing factors of the disease. In approximately 3% of the patients, the lesions on the mucosa can transform into squamous cell carcinoma. Some cases of lichen planus affect the scalp or nails exclusively.
WHAT CAUSES LICHEN PLANUS?
The exact cause of lichen planus remains unknown or idiopathic. Besides its correlation with family history, certain drugs also do seem to trigger the condition. Among them we can find: anxiolytic drugs, antipsychotics, gold, anti – malaria drugs, quinidine, thiazide diuretics as well as angiotensin – converting – enzyme inhibitors. Moreover, it has been noted that lichen planus is more common in people suffering from various autoimmune diseases e.g. vitiligo, systemic lupus erythematosus, conditions of the thyroid gland, and inflammatory bowel disease.
SIGNS AND SYMPTOMS
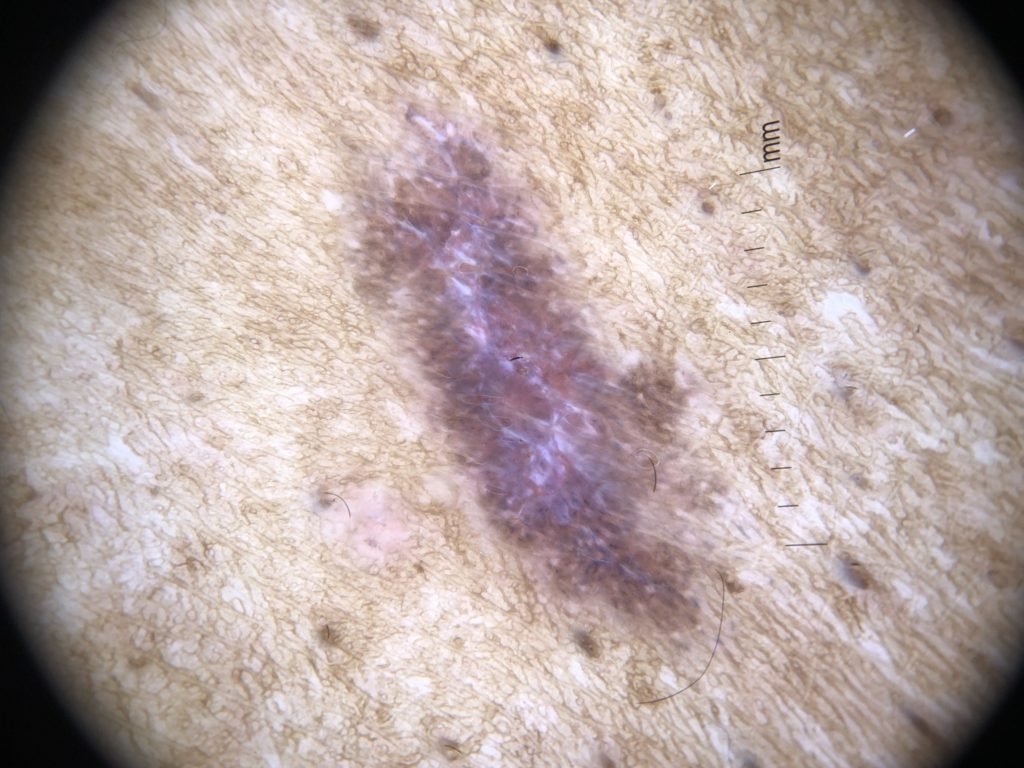
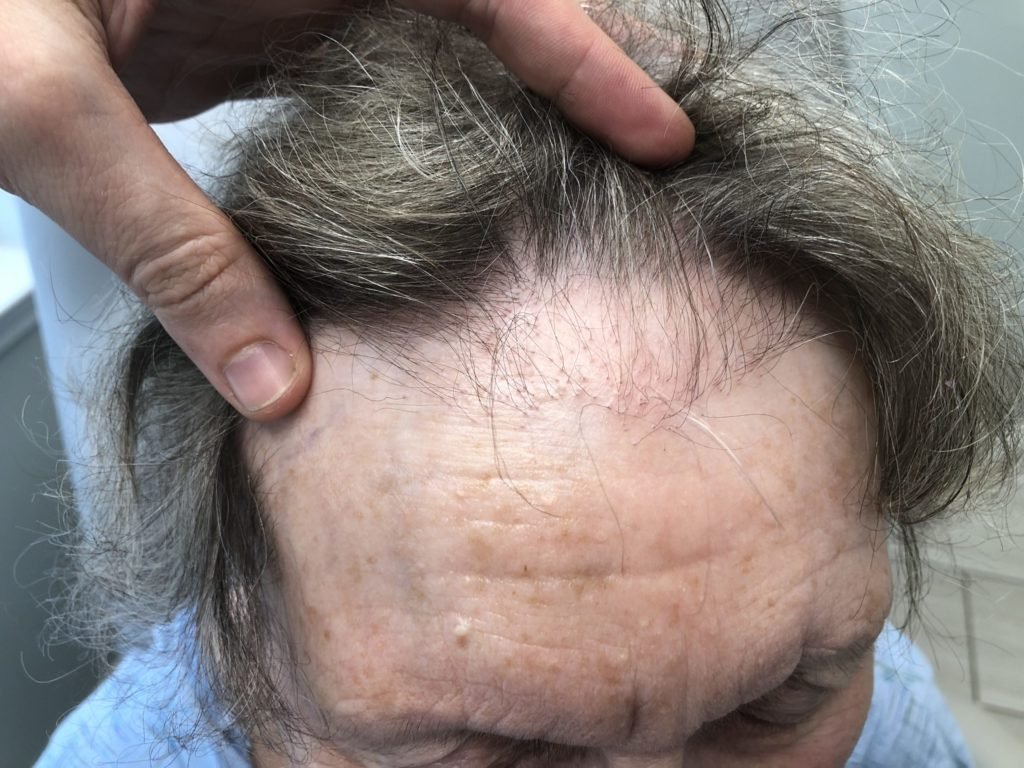
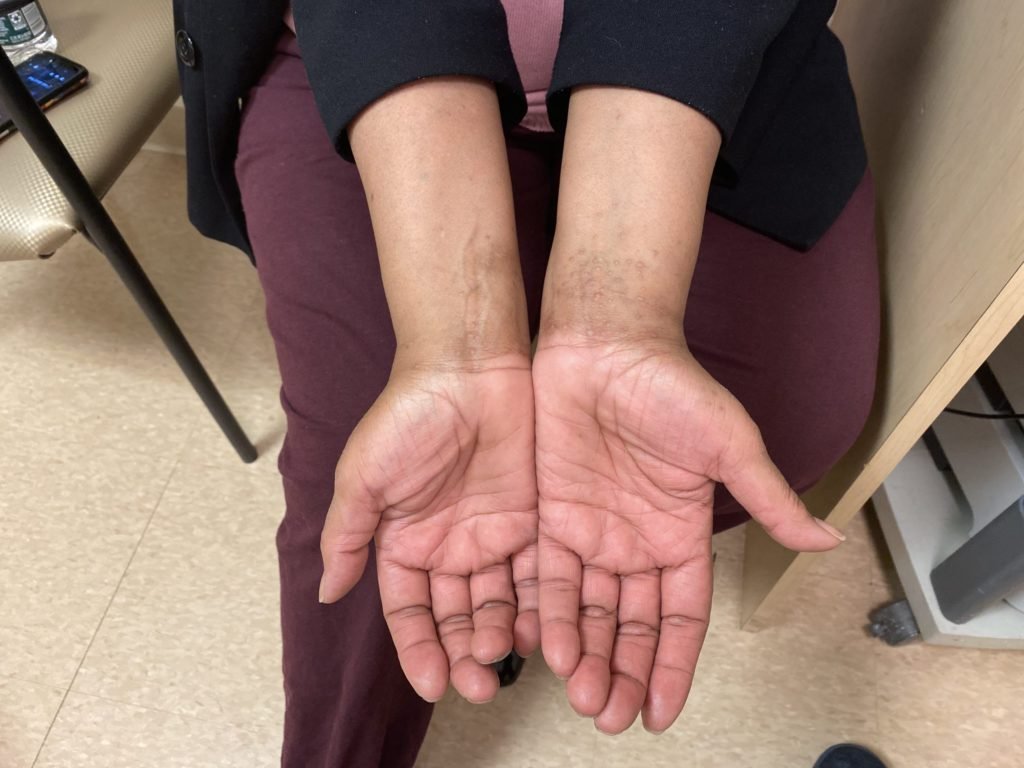
The primary lesion in lichen planus is a polygonal, flat – topped, purple papule with so – called Wickham’s striae on its surface – white fine lines which become visible when in contact with mineral oil. The lesions are most commonly located on the flexor surfaces of one’s wrists, forearms, ankles and groin as well as in places of previous mechanical injury (Koebner’s sign). What is characteristic of the condition is itch and discomfort. Mucosa are also very frequently affected, especially in one’s oral cavity. There, typical white tree – shaped, branched lesions can be seen. When lichen planus affects the nails, they usually get covered with characteristic linear grooves. The nail may also darken, thicken or be completely lifted off the nail bed, a condition called onycholysis. With time, the lesions on the skin thicken and become hypertrophic due to excessive cell proliferation. Many time, the lesions will leave dark marks called “hyperpigmentation” behind. Sometimes, the rash spontaneously disappears on its own after 1 – 2 years, however, therapy is often requires to control the symptoms. On the scalp, Lichen planus can cause hair loss both diffusely, as well as in a band across the front of the hairline and eyebrows (Frontal Fibrosing Alopecia).
"Phototherapy is a very effective option in the treatment of lichen planus. It is well - tolerated, non – invasive, and can be safely repeated."
PHARMACOLOGICAL THERAPY
Pharmacological therapy is an effective option in the treatment of lichen planus. In this case, first choice treatment is high potency topical steroids – e.g. clobetasol (Clobex®), mometasone (Elocon®) or fluocinonide (Lidemol®). Triamcinolone (Kenalog®) injections are an effective method of treating thickened or picked areas. Second choice pharmacological treatment is topical tacrolimus (Protopic®). For cumbersome itching, oral antihistaminics (hydroxyzine, loratadine) are often prescribed. In more severe or resistant instances, oral prednisone, acitretin, azathioprine, cyclosporine or hydroxychloroquine are to be considered. Pennsylvania Dermatology Specialists will determine the most suitable therapy in your individual case to address your concerns.
PHOTOTHERAPY THERAPY IN LICHEN PLANUS
Phototherapy is a very effective option in the treatment of lichen planus. It is well – tolerated, non – invasive, and can be safely repeated. During a session, narrowband UVB light is used. This term refers to a specific sort of ultraviolet light, with a particular wavelength of 311-312 nm. The studies have shown that this kind of radiation provides the best results in clearing various skin conditions. It has also been proven safe in terms of skin cancer – there exists no proof that phototherapy increases the risk for development of this disease. In most of the cases, a common treatment plan consists of 2-3 treatments a week over several weeks, and Pennsylvania Dermatology Specialists will personalize your therapy parameters for the best possible effects.
