Actinic Keratoses
Actinic keratoses are some of the most common lesions discovered during skin exams, and are often referred to as ‘pre-cancers’. In dermatology, we simply call them ‘AKs’.
So, what exactly is the risk? That’s a very good question, and one which has many answers. The estimated rate of transformation from AK to SCC ranges from less than 1% to well over 10%. The problem in providing an exact rate is that so many factors play a role. These include a patient’s age, immune status, history of skin cancer, and current level of UV exposure.
Regardless of the exact risk, AKs can turn into skin cancer, and the general recommendation is that it is safer to treat them than it is to monitor them.
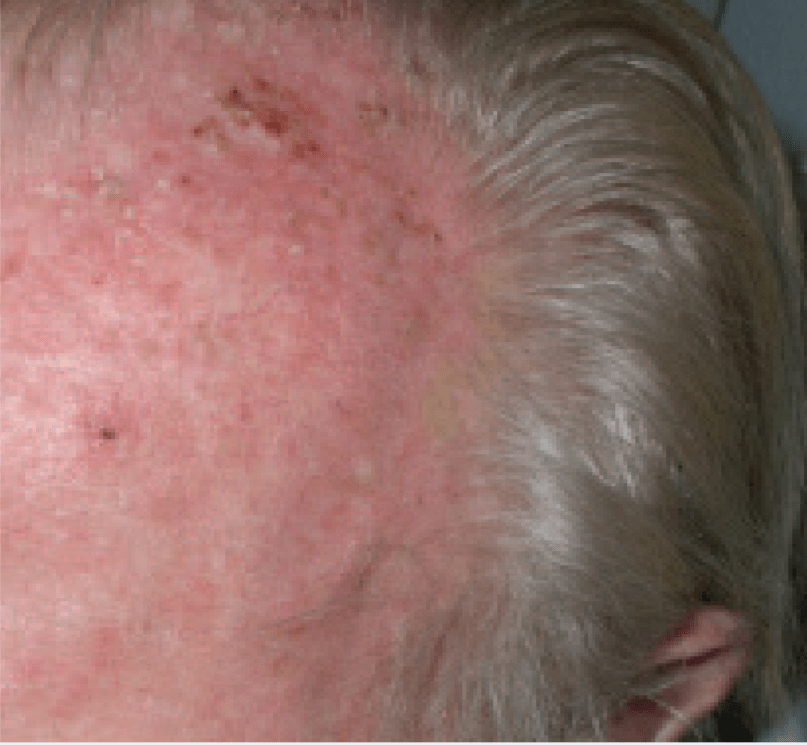
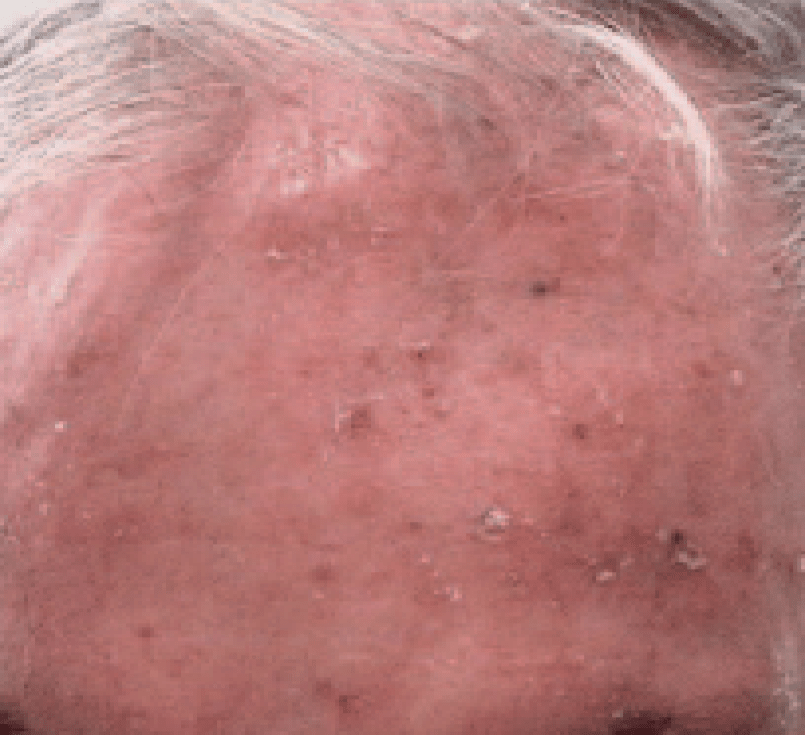
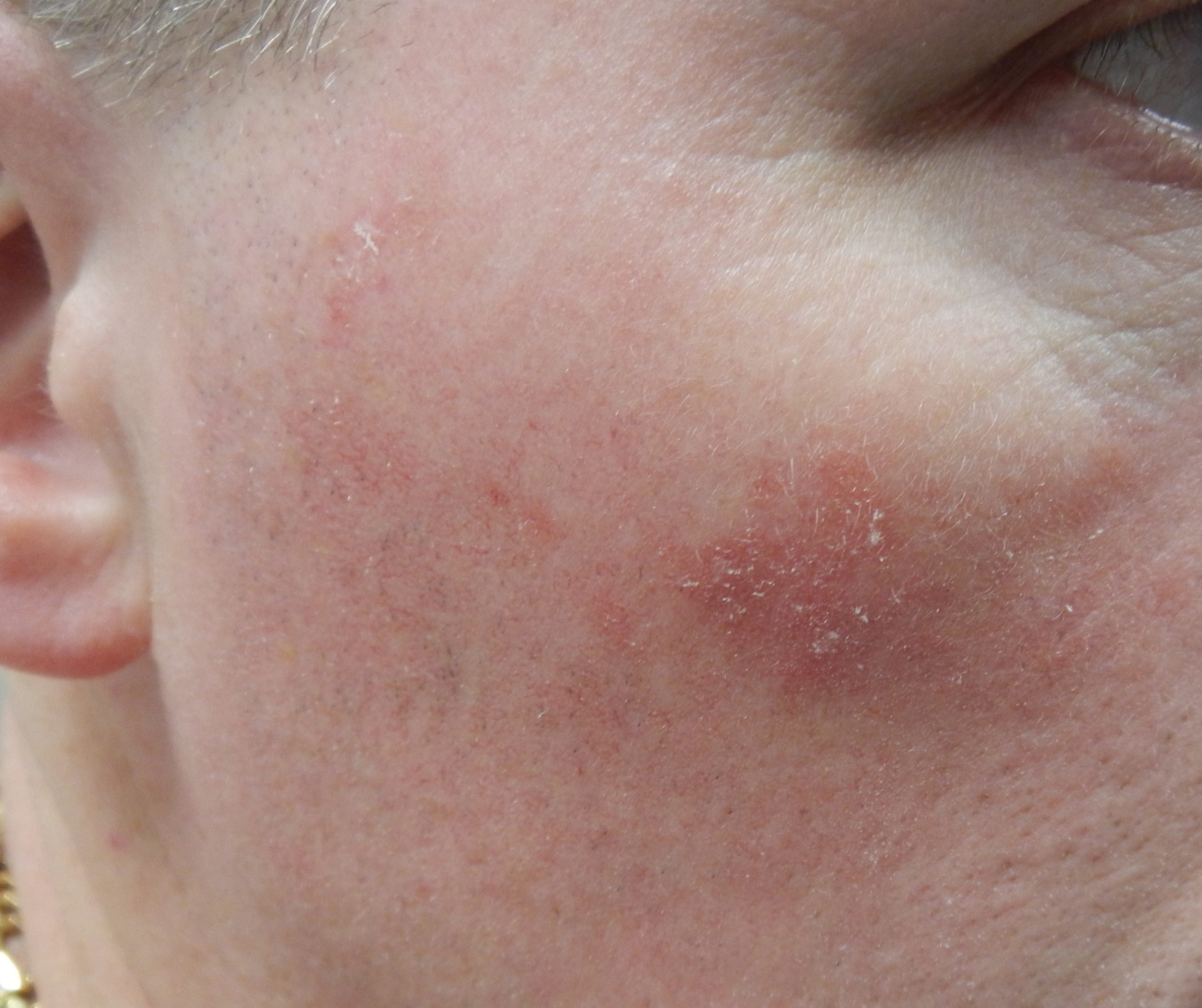
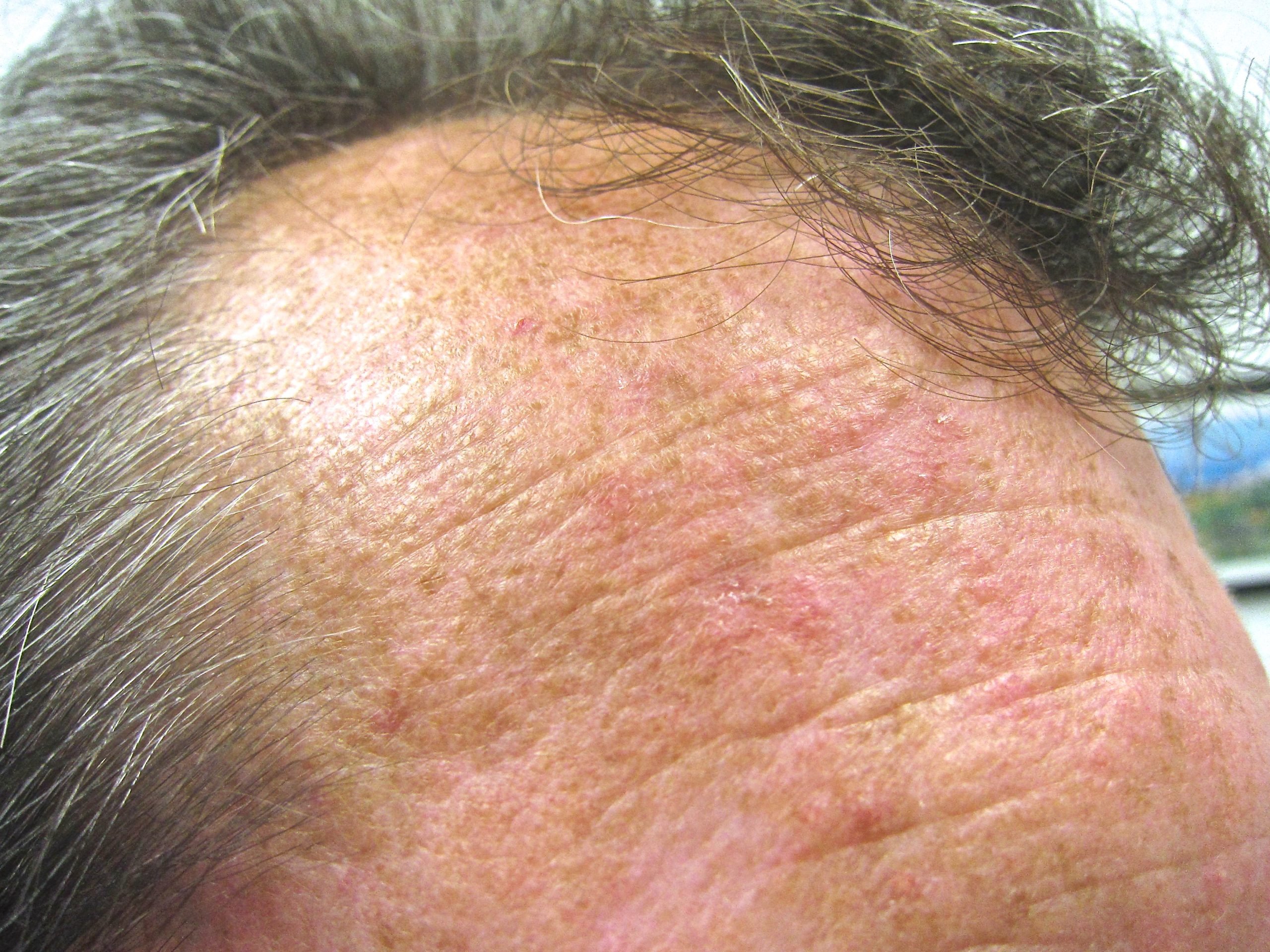
AKs result from damage caused by ultraviolet (UV) light – found in both natural sunlight as well as tanning bed lamps. The UV light changes the cells in a way which causes them to ‘grow too fast for their own good.’ The affected epidermis doesn’t mature normally and tends to appear red, feel rough and may even be sensitive to the touch.
The reason they’re called ‘pre-cancers’ is because the majority of squamous cell carcinomas (SCC) arise from AKs.
That said, the majority of AKs do not turn into SCC.

Treatment
For a limited number of AKs, ‘cryosurgery’ is the most common treatment method. In this treatment, liquid nitrogen is applied to the AK so that it is essentially ‘frostbitten’. This causes the lesion to become inflamed and within a few weeks will peel away. Like any treatment, there are a few disadvantages to this approach.
The first downside to cryosurgery is that each application of liquid nitrogen hurts a little, causing the treatment sites to feel sensitive both during the treatment and up to a few days thereafter. Freezing can also damage otherwise healthy pigment cells, causing some treatment sites to remain permanently appear lighter in color than the surrounding skin. Last but not least, cryosurgery works best as a ‘spot treatment’. That is, if a patient has a limited number of AKs, then freezing can work well. If there are many AKs grouped together over larger areas, there are alternatives which might be a better choice.
These other approaches are often referred to as ‘field’ treatments. They’re given this name because instead of just treating individual lesions as freezing does, they can treat entire areas (‘fields’) of affected skin such as the face, forearms or hands. The two most common ‘field treatment’ methods are that of using a topical prescription at home, or through a procedure performed in the doctor’s office.
The topical prescription method involves applying a cream to the AKs. There are several such creams available and they are used anywhere from a few days up to several weeks. The main advantage of using such a cream is that doing so allows multiple lesions to be treated at once. The creams also primarily target the abnormal cells, causing minimal damage to healthy skin, so the risk of scarring is much less than it is with freezing.
The main disadvantage to using one of these topical prescriptions is that during the treatment process, the affected areas will become red and inflamed – especially toward the end of treatment.
Patients treating a highly visible area (such as the face) would need to consider work and social obligations before committing to this approach. Finally, these creams can be expensive. Insurance generally provides coverage, but copays and deductibles can result in significant out-of-pocket costs.
The alternative to using a topical prescription at home is a procedure performed in the clinic called photodynamic or ‘red/blue light’ therapy. This procedure is performed by first applying a liquid called aminolevulinic acid (ALA) to the affected areas. The ALA is preferentially absorbed by the rough, scaly cells of the typical actinic keratosis. After allowing time to absorb, the skin is then exposed to a special high-intensity lamp for under 20 minutes, which activates the ALA to destroy the atypical cells. Like the prescription creams previously mentioned, the ‘red/blue light’ treatment also causes redness and inflammation. However, with ‘red/blue light’ treatment the redness begins right away (the day of the treatment) and generally resolves within 5-7 days (rather than lasting weeks as with the cream). Finally, because it’s a procedure rather than a prescription, insurance may pay be more likely to pay for ‘blue light’ since medication coverage isn’t generally required.