Seborrheic Dermatitis
Seborrheic dermatitis (‘seb derm’) is a skin condition characterized by inflammation and flaky scaling throughout what are traditionally ‘oil-prone’ areas of the body. In fact, the medical term sebum refers to the oil produced by our skin, so the word seborrheic essentially means ‘oily’. In adults, affected areas can include the scalp, forehead, eyebrows, ears, nasal creases, and mid-chest. It’s even known to occasionally affect the scalp of young children, where it’s referred to as ‘cradle cap’.
Many patients with seborrheic dermatitis don’t even realize that they have a treatable skin condition. When limited to the scalp, it’s frequently dismissed as ‘dandruff’. On the face, many simply think they have dry skin. Apart from its scaly appearance, itching can also be a problem.
So what causes it?
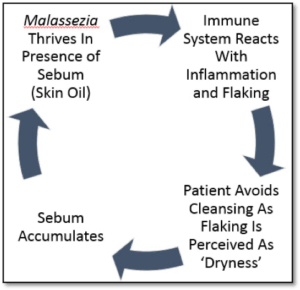
While a number of factors influence seborrheic dermatitis, the most significant seems to be a naturally-occurring yeast known as Malassezia. Even though it can be found to a degree on everyone’s skin, those with ‘seb derm’ thought to be sensitive to either its presence alone or perhaps the toxins it produces. As seen here, Malassezia transforms what should be oily skin into the flaky rash we recognize as seborrheic dermatitis.
Although no ‘cure’ is available, flares of seborrheic dermatitis are generally very easy to control with the right treatment approach. Because of the role of Malassezia, yeast-controlling medications provide a good starting point. In fact, the active ingredients within most dandruff shampoos are those which kill yeast.
For some patients, though, other factors are at play and controlling Malassezia alone isn’t enough. When this happens, additional treatment options include mild topical steroids or nonsteroid creams or lotions. Your dermatologist will review these options and provide recommendations based on your specific needs and response to prior treatment methods.
