Hidradenitis Suppurativa
WHAT IS HIDRADENITIS SUPPURATIVA?
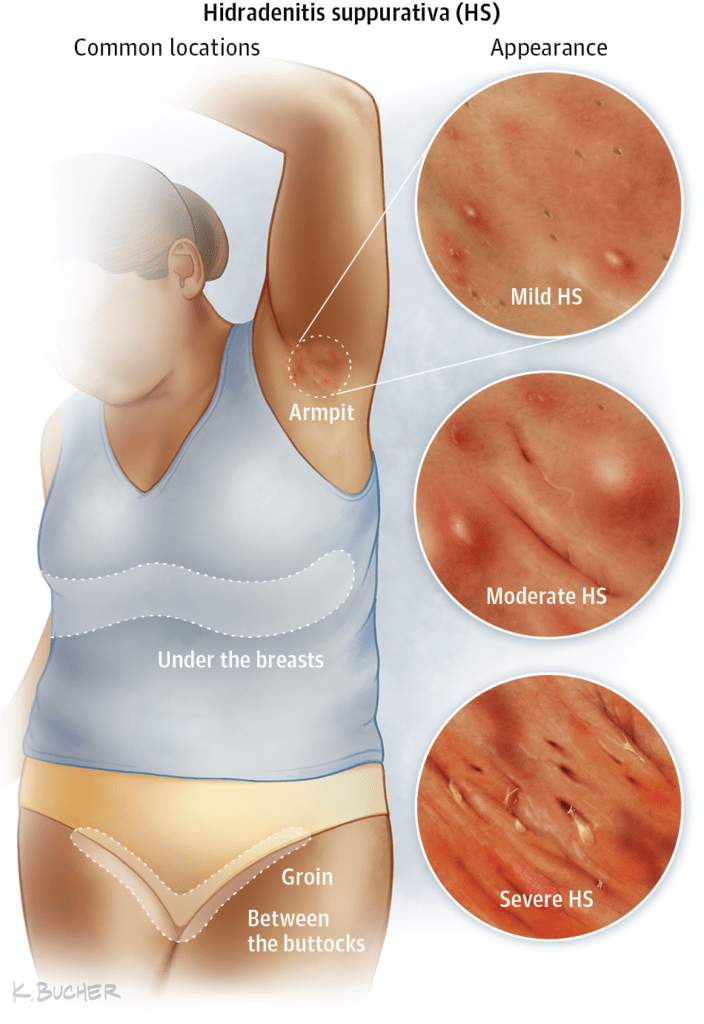
Hidradenitis suppurativa, or acne inversa, is a chronic inflammatory skin disorder which affects the skin folds: mostly armpits, groins, anogenital region and under the breasts area. In its developed form, the lesions appear as painful nodules with a tendency to scarring and abscess formation. Its recurrent and progressive course can drastically influence the patient’s mental and physical wellbeing.
EPIDEMIOLOGY
The disease is definitively more common in women than in men. It is most active between the ages of 20 and 40 years, often starting right after puberty and subsiding with the onset of menopause. Besides the associated hormonal changes, other risk factors have been noted including family history, smoking, obesity, inflammatory bowel disease as well as genetic predisposition. No association with diabetes, bad hygiene, depilation, deodorant usage or regular acne vulgaris has been observed.
WHAT CAUSES HIDRADENITIS SUPPURATIVA?
Until this day, the exact cause of the disorder remains unknown. It is believed that acne inversa primarily affects the hair follicles that get clogged due to local hyperkeratosis. This process elicits intense inflammatory response which later can spread to deeper skin layers as well as impair or completely destroy apocrine sweat glands.SIGNS AND SYMPTOMS
Symptoms of hidradenitis suppurativa closely reflect its progressive course described in the previous paragraph. Firstly, clogging of the hair follicles gives rise to the formation of multiple comedones, pustules and papules, which can strongly resemble regular acne vulgaris. Then, as the inflammatory response spreads to the deeper skin layers, pus – filled abscesses occur. Further progression of the disease entails the formation of painful, confluent nodules which look like furuncles or boils. They, on the other hand, lead to scarring and development of sinuses – tunnels or cavities connecting to the skin or mucosal surface.GENERAL DAILY MEASURES
- Smoking cessation – it can lead to improvement within a few months
- Loose fitting clothing – it will not further irritate the affected skin
- Weight loss via regular physical activity and implementation of a healthy, balanced diet
- Using only gentle, fragrance-free cosmetics
- Oral over – the – counter analgesics for pain control, such as paracetamol or ibuprofen
PHARMACOLOGICAL THERAPY
HS can be treated with and triamcinolone (Kenalog®) injections, which have been proven effective when dealing with small cysts. Topical options include antibiotics like clindamycin with benzoyl peroxide, antiseptics, topical steroids, and topical resorcinol.
Regarding oral therapy, the antibiotics from the tetracycline or macrolide groups are used including tetracycline, doxycycline, minocycline, and azithromycin. Hormonal medications like antiandrogens (Drospirenone, Spironolactone, Finasteride), insulin sensitizing medications (Metformin), and supplement options are also available treatments. In more resistant cases, immunomodulatory drugs seem to be helpful including short – term systemic corticosteroids, as well as biological TNF – α inhibitors: Adalimumab (HUMIRA®), which is FDA-approved. Infliximab (REMICADE®) and Ustekinumab (Stelara®) have also shown benefit. Pennsylvania Dermatology Specialistsare experts in treating Hidradenitis Suppurativa, and will adjust the pharmacological therapy specially to your personal needs.
SURGICAL THERAPY
Surgical therapy is an effective treatment for HS, but it is often deferred due to its invasive character. During the procedure, the affected glands and tissue with a small margin of healthy skin (for relapse prevention) are being removed, either with the usage of a laser or a scalpel. Pennsylvania Dermatology Specialists will assess the best possible approach in your individual case.HS can be treated with numerous topical, oral, injectable, and even device based treatments. Surgery is available for patients with severe disease not amenable to more simple measures. Through a combination effort, we can make improvements in even the most difficult cases of hidradenitis suppurativa.
Although it can be difficult to treat, it is possible to get significant improvement of Hidradenitis Suppurativa with treatment. These patients were treated with Humira ®.