We often treat our skin like the wallpaper of our lives, noticing its color or texture only when the light hits it just right. It’s a seamless, resilient boundary that manages an incredible amount of biological heavy lifting without ever asking for a day off. Yet, this quiet guardian is constantly reacting to an invisible environment of radiation and time. Understanding the rhythm of its changes is less about vanity and more about maintaining the integrity of our most vital armor.
Establishing the Annual Baseline
For most adults, the standard recommendation for a professional skin check is once every twelve months. This annual milestone allows an expert to establish a clear baseline for what’s normal for your unique skin. Think of it as a proactive maintenance check that ensures nothing is shifting beneath the surface without being noticed. Early detection remains the most powerful tool available for successfully managing your long term health.
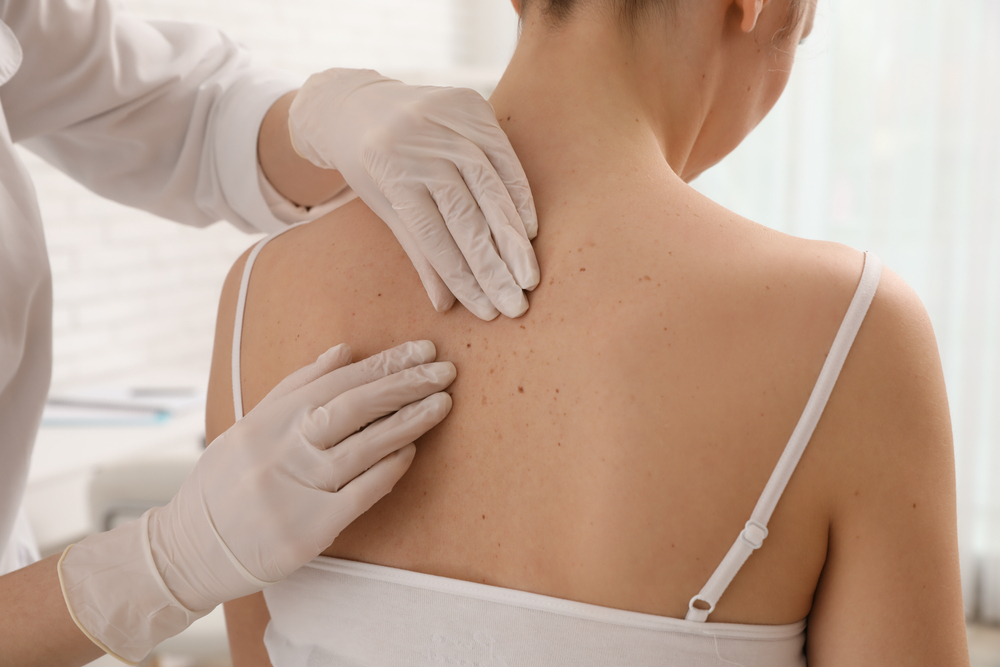
During this yearly visit, a specialist will examine your skin from head to toe to identify any suspicious growths. These appointments are designed to find cancers like melanoma before they have a chance to spread. Many patients find that the peace of mind following a clear exam is well worth the time spent in the office. Regularity is the key to ensuring that your health history remains a boring one.
If you have never had a professional exam, your first visit will serve as the foundation for all future screenings. A dermatologist in Montgomery County or elsewhere will document the location and appearance of your existing moles and freckles. They will also discuss your lifestyle and past sun exposure to help tailor your future care. This initial data is essential for identifying subtle changes that might occur over the following years.
Understanding Individual Risk Factors
Certain biological and environmental factors can significantly change how often you should walk through the clinic doors. If you have a personal history of skin cancer or multiple atypical moles, your schedule will likely look different. Those with a family history of melanoma often require more frequent surveillance to stay ahead of potential issues. Your natural skin tone and the amount of lifetime sun exposure also play a major role in determining your personal risk.
The timeline for your next visit depends heavily on your unique biological blueprint. People with fair skin, light eyes, and freckles often burn more easily, which increases the likelihood of DNA damage. However, individuals with deeper skin tones still face risks, often in areas like the palms or soles of the feet. A personalized consultation helps bridge the gap between general guidelines and your specific medical needs.
Consistency in your screening schedule is particularly important if you have experienced several blistering sunburns in the past. These early life events can have a cumulative effect on your skin cells decades later. A specialist can help you understand how these history markers influence your current health. By staying vigilant, you can counteract the risks associated with your past environment.
Monitoring Changes Between Appointments
While professional checks are vital, your own observations play a critical role in the detection process. Performing a monthly self exam allows you to become the foremost expert on your own skin. You are the most likely person to notice if a mole has changed its shape or if a new spot has suddenly appeared. This partnership between patient and provider is the most effective way to maintain a safe environment.
- Stand in front of a full length mirror in a well lit room to check your front and back.
- Raise your arms to examine your right and left sides thoroughly from top to bottom.
- Use a hand mirror to check the back of your neck and scalp by parting your hair.
- Examine your back, buttocks, and the back of your legs carefully using the hand mirror.
- Check your hands, palms, fingernails, and the spaces between your fingers for any changes.
When you perform these checks, keep a close watch for the “ugly duckling” sign. This refers to a spot that looks significantly different from all the other moles on your body. It might be darker, lighter, or have a more irregular border than its neighbors. If you find a spot that stands out, it’s always better to have it evaluated sooner rather than later.
Advanced Surveillance for High Risk Profiles
Individuals with a higher risk profile often need screenings every three to six months. This frequency ensures that any rapidly changing cells are caught in their earliest and most treatable stages. Following a specific plan for skin cancer treatment in Southampton that’s created by a specialist is the best way to manage ongoing concerns. Consistent monitoring reduces the anxiety that often comes with a history of cumulative sun damage.
| Risk Category | Recommended Frequency | Primary Goal |
| Average Risk | Every 12 Months | Baseline Monitoring |
| History of Basal Cell | Every 6 to 12 Months | Recurrence Check |
| History of Melanoma | Every 3 to 6 Months | Intensive Surveillance |
| Atypical Mole Syndrome | Every 6 Months | Evolution Tracking |
For patients with a very high number of moles, whole body photography might be recommended as an additional tool. This process involves taking high resolution images of your skin to serve as a permanent visual record. During future visits, the dermatologist can compare your current skin to these photos to spot new arrivals. It’s an incredibly effective way to manage complex cases without performing unnecessary biopsies.
Another specialized tool used during these exams is dermatoscopy. This technique allows your doctor to see structures within the skin that are invisible to the naked eye. It uses polarized light and magnification to reveal the intricate patterns of a mole. This level of detail provides an extra layer of security during every high risk visit.
Specialized Treatments for Skin Cancer
When a screening reveals something concerning, advanced surgical options like Mohs surgery become vital for treatment. This precise technique removes cancerous cells layer by layer while preserving as much healthy tissue as possible. It’s particularly effective for areas where appearance and function are high priorities for the patient. A specialist will guide you through the process if this level of care is required.
- Mohs surgery offers the highest cure rate for most common skin cancers found today.
- The process involves immediate microscopic examination of removed tissue for maximum accuracy.
- Specialists can ensure all margins are clear during a single visit to the office.
- This method minimizes scarring and promotes faster healing for delicate areas like the face.
Treatment plans are always personalized to the specific type and location of the cancer. Some early stage issues can be managed with topical therapies or simple excisions. More complex cases might involve a multidisciplinary team of experts to ensure the best outcome. The goal is always to eradicate the cancer while maintaining your quality of life.
Modern dermatology has made incredible strides in making these treatments as efficient as possible. Most procedures are performed in an outpatient setting with local anesthesia. This allows you to return to your normal routine with minimal disruption. Knowing that advanced options are available can make the screening process feel much less daunting.
Debunking Common Screening Myths
Many people believe that they only need to worry about spots that are dark or raised. In reality, some forms of skin cancer can look like a simple dry patch or a pearl colored bump. Others think that a tan provides a safety net against damage, but any change in color indicates injury. Regular screenings help debunk these myths by providing professional clarity for every unique skin type.
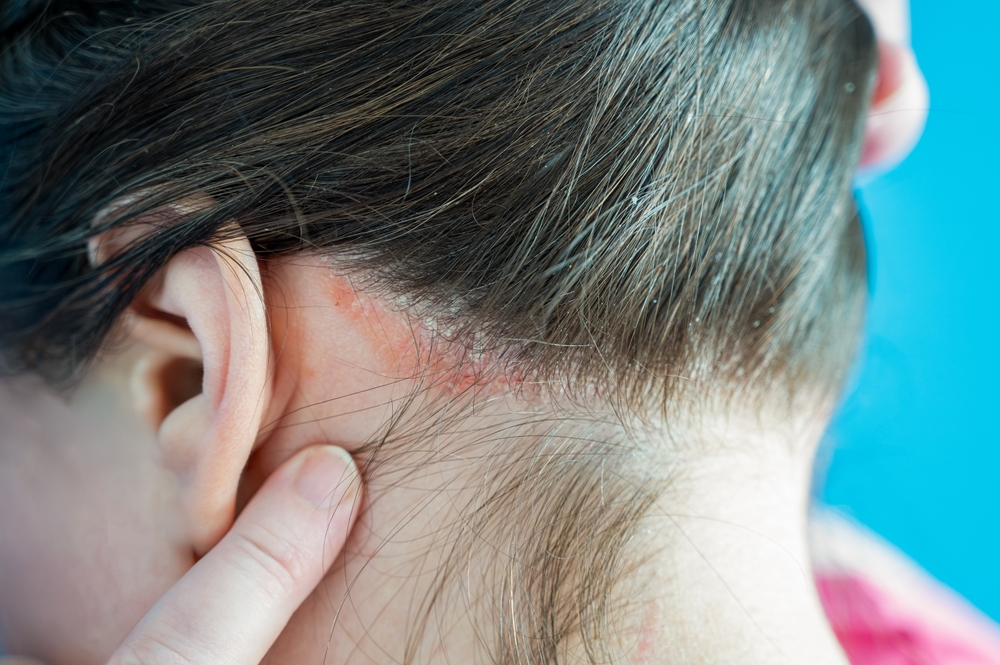
One common misconception is that skin cancer only occurs on parts of the body that see the sun. Melanoma can actually develop in hidden areas like the scalp, under the nails, or even between the toes. This is why a professional total body skin exam is so different from a quick look in the mirror. Professionals are trained to check every hidden crevice where a silent issue might be hiding.
Age is another factor that is often misunderstood in the context of skin health. While the risk of most skin cancers increases as we get older, melanoma is one of the most common cancers in young adults. This means that starting a regular screening habit in your twenties is a wise health decision. No matter your age, your skin deserves the same level of attention as the rest of your body.
Preparing for Your Professional Visit
The team at Pennsylvania Dermatology Specialists approaches every examination with a focus on precision and patient comfort. They understand that a skin check can feel vulnerable, so they prioritize clear communication throughout the entire process. By utilizing the latest diagnostic technology, they can track subtle changes in your skin over several years. This continuity of care is what makes a professional relationship so valuable for your wellness.
- Remove all nail polish from your fingers and toes before your scheduled appointment.
- Avoid wearing heavy makeup so the provider can see your facial skin clearly.
- Perform a quick self check at home to identify any spots you want to discuss.
- Bring a list of any personal or family history regarding your skin health.
- Wear clothing that is easy to remove and put back on after the exam.
During the exam, do not be afraid to ask questions about specific spots that have bothered you. Mention if a spot has been itchy, painful, or if it has bled recently. Your input provides context that helps the dermatologist make more accurate assessments. Open dialogue ensures that you leave the appointment feeling informed and confident in your health plan.
The exam itself is usually quite fast and typically takes less than fifteen minutes. You will be asked to wear a gown to allow for a full inspection of your skin surface. The provider will move systematically from your scalp down to the soles of your feet. This thorough approach is designed to catch everything from common spots to rare conditions.
Daily Habits for Long Term Protection
Maintaining your skin health also involves daily habits that complement your professional screenings. Protective measures are the first line of defense against the cumulative effects of ultraviolet radiation. Small choices made every day add up to a significant reduction in your lifetime risk. Consistency in these habits is just as important as the frequency of your doctor visits.
- Apply a broad spectrum sunscreen with at least SPF 30 every single day of the year.
- Seek shade during the peak hours of the sun between mid morning and late afternoon.
- Wear protective clothing like wide brimmed hats and sunglasses whenever you are outdoors.
- Avoid all forms of indoor tanning beds which significantly increase your lifetime cancer risk.
Proper sunscreen application involves using enough product to cover all exposed areas. Most adults need about an ounce, or a full shot glass, to cover their entire body. It’s also important to reapply every two hours if you are spending time outside or swimming. This proactive approach keeps your skin resilient against the elements.
Remember that sun damage can occur even on cloudy or cold days. Ultraviolet rays can penetrate through clouds and reflect off surfaces like water or snow. Building these protection habits into your daily routine makes them second nature. When you combine daily protection with regular screenings, you are taking the most comprehensive approach to skin health.
Putting Your Mind and Skin at Ease
Taking the time to check your skin is a meaningful gift to your future self that pays dividends in peace of mind. Regular screenings with the compassionate team at Pennsylvania Dermatology Specialists ensure that you are never facing your skin health journey alone. Reach out to our experts today to establish your personalized screening schedule and protect your most visible asset.